
For years, Jennifer Miller, 55, of Carleton, Michigan, was a problem sleeper, snoring and gasping through the night. Because she struggles with PTSD from the crash that gave her a T10 spinal cord injury and isn’t the biggest fan of doctors and hospitals in the first place, she put off seeking treatment for her sleep issues. “I didn’t say anything for a long time,” the United Spinal Association member says. But that changed a year ago, on a night that literally left her speechless.
“I couldn’t find breath and I couldn’t say anything. I couldn’t wake up my fiancé. I had to sit up and … kept trying to breathe in and nothing was happening,” Miller says. When at last she could draw a breath, her sleep issue had new urgency. “It scared me [and] prompted me to actually speak to the doctor.”
Miller’s overnight scare is a dramatic and extreme example of sleep apnea, the interruption of breathing during sleep. Sleep apnea is experienced by between 9% and 38% of the general population, according to one study, but within the SCI community it can be much higher.
My introduction to sleep apnea wasn’t as dramatic as Miller’s, but certainly memorable. As someone with multiple sclerosis who functions much like a high-level quad, my daily naps had led my neurologist to order an overnight sleep study. When he had the results, he left a dire voicemail … on a Saturday afternoon: “Mr. Mohler, you have very severe sleep apnea.” My sleep study report read like a horror movie script. In six hours, I had 327 full or partial breath stoppages, with full stoppages averaging 45 seconds each. In short, I wasn’t breathing for 2.5 of the six hours. My blood-oxygen level — considered healthy in the 90% range and severe below 80% — nose-dived to 62%. “At least we know you have a healthy heart,” he said later, “because if you didn’t, you’d be dead.”
Fortunately, sleep apnea can be effectively treated with common bedside medical devices called continuous positive airway pressure machines (CPAP) or bilevel positive airway pressure machines (BiPAP), both of which use a face mask to direct pressurized air into the airway to help keep it open and functioning.
Unfortunately, the masks and tubing come in various degrees of cumbersome, ranging from annoying and uncomfortable to full-on alien-abduction vibes, with strange, elephant-like hoses and face-sucker masks. In looks, they bring to mind the Alien movies, and they can sound like Darth Vader gasping for air.
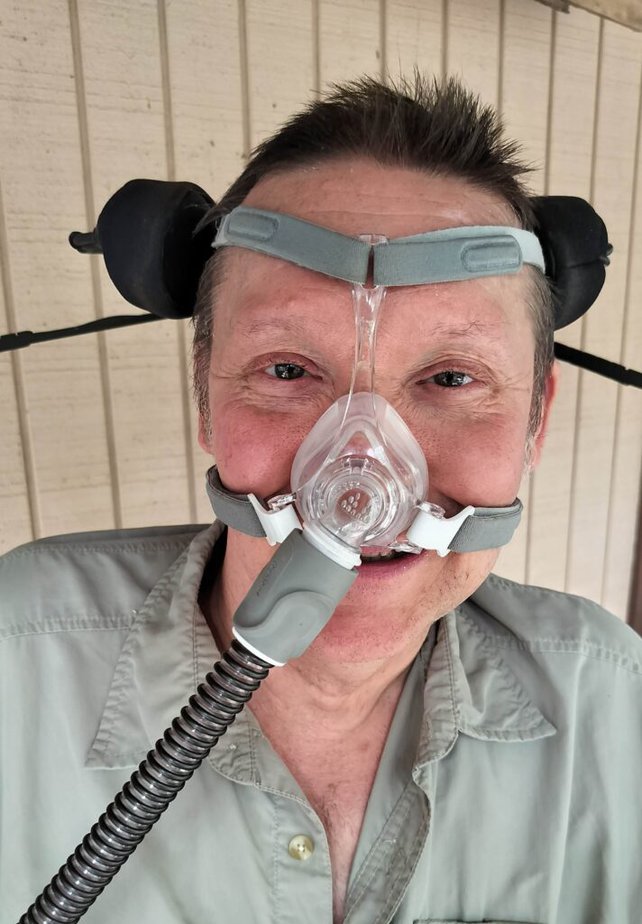
Those starting CPAP and BiPAP therapy must make significant bedtime adjustments that many never get past: At a time of day for winding down, it’s a lot to grapple with to bring a hyperventilating face-snake into your daily relaxation routine. Accessibility issues can make the learning curve even steeper, so those with disabilities must bring their creativity and patience to unlock what can be a lifesaving treatment.
Sleep Apnea, CPAP/BiPAP and SCI
Sleep apnea occurs when the muscles near the back of the throat relax, allowing the soft tissue there to obstruct or block the airway; or, less commonly, when the brain fails to send signals to the breathing muscles. Uncorrected, sleep apnea often leads to fatigue and risks for high blood pressure, heart problems and type 2 diabetes. Chronic poor sleep, in turn, has been linked to shorter lifespans.
CPAP applies a consistent air pressure, while BiPAP machines offer different pressures for in-breaths and out-breaths, so users don’t feel they are fighting the machine to breathe out. Both types offer adjustable pressure and often climate controls like a humidifier or temperature adjustment.
CPAP/BiPAP therapy is effective in decreasing sleep apnea at night and sleepiness during the day, but many users drop out, citing discomfort with gear, claustrophobia, and dryness in the mouth and nasal passages.
It’s a lot to grapple with to bring a hyperventilating face-snake into your daily relaxation routine.
A prominent expert who treats wheelchair users in both clinical and research settings finds a relationship between higher-level SCIs and sleep-disordered breathing such as sleep apnea. Dr. Abdulghani Sankari, with more than 15 years as a researcher and pulmonologist, practices sleep medicine at Henry Ford Providence Hospital and the DMC DRH Sleep Disorders Center. The title of one of his published studies speaks for itself: “Tetraplegia Is a Risk Factor for Central Sleep Apnea.”
“At T6 and above, the prevalence [of sleep-related breathing problems] is above 80%,” Sankari says. “It is higher in the cervical [injuries] up to C4, … up to 90%.” Sleep-disordered breathing shows up at much greater rates in those with cervical and upper thoracic-level SCIs than in paraplegics and those with lumbar SCIs, who have rates similar to the general population. Reasons for the higher rates among those with higher-level injuries are unknown, but researchers are looking into sleep apnea’s connections to wider neck circumferences, traumatic cervical injuries and decreased circulation, among other possibilities.

A frustrating irony Sankari faces with treatment is that those affected by sleep apnea often don’t realize it until after they start using CPAP/BiPAP, because they are attributing their fatigue to other problems going on at the same time. “They have pain issues, they have urinary issues, they have cardiovascular issues … They’re tired and not able to sleep well because of all these factors,” he says, “so they don’t recognize that there are other reasons … [why] they feel tired during the day.” CPAP/BiPAP typically addresses manifested symptoms like daytime listlessness, waking up unrefreshed from sleep, and unexplained chronic pain. CPAP/BiPAP also helps improve aspects of sleep-affected cognition: memory, forgetfulness, attention span and intellectual abilities like troubleshooting problems effectively.
Letting problems like these linger can even cause one’s condition to worsen. “The frequent interruption of breathing at night leads to what we call chronic intermittent hypoxia, so the body is exposed to low levels of oxygen, and that produces byproducts of inflammation and waste that [aggravate] symptoms on the central nervous system,” Sankari says.
Adapting to Life Behind the Mask
Todd Stabelfeldt saw a CPAP machine on a TV news-magazine program in 1990 and told his mom he needed one. The precocious 11-year-old, a C4 quadriplegic, had been cranking a fan on high in his face every night because he couldn’t breathe. Three years later, Stabelfeldt, now 46 and CEO of C4 Database Management in Seattle, was diagnosed with sleep apnea. “My doctor said, ‘Well, you were trying to make your own CPAP machine, basically.’”
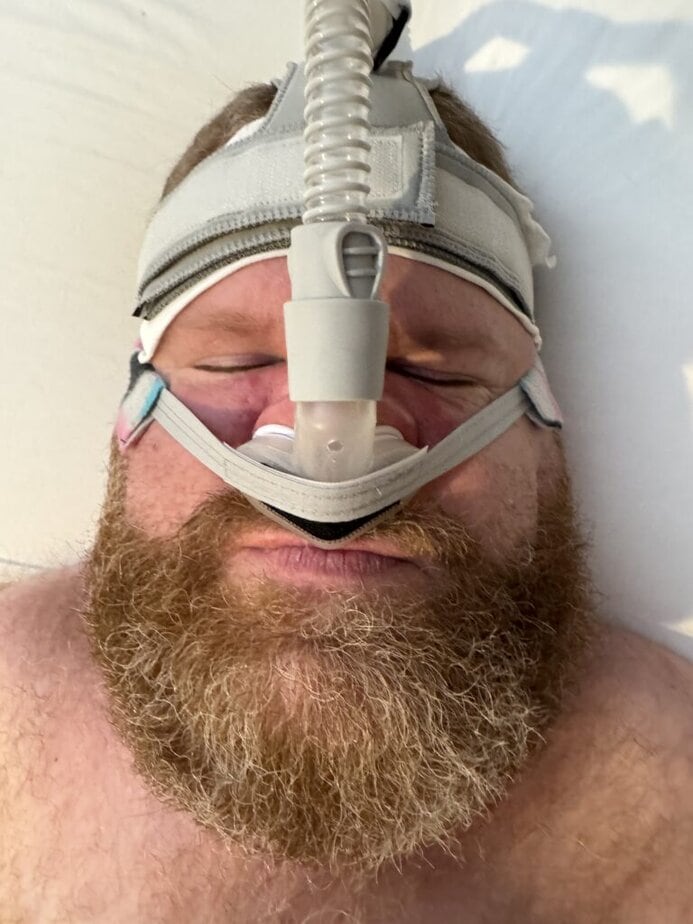
Stabelfeldt tried a BiPAP machine during his sleep study and never went back. “I could totally tell a difference. … It was the best sleep I’ve ever had in my life,” he says.
While Stabelfeldt made a successful jump to BiPAP in one night, my adjustment to CPAP was neither smooth nor fast. An unhelpful provider and a pulmonologist met my accessibility questions with blank stares. I got saddled with an oversized mask that covered nose and mouth and made me feel like Jacques Cousteau. It also took away my ability to use voice access when I woke up, which freaked this quad out. Unsurprisingly, that machine wound up in a closet, collecting dust. Likewise, Miller’s transition to CPAP was marred by indifferent, uncommunicative initial support from providers.
Finding a better neurologist and mask were key to my getting a handle on things. There are several mask styles available, and I settled on a smaller one that fits over the nose. With the mantra “more oxygen, more energy, more strength,” I pushed myself to endure longer sessions each night. I progressed from watching the clock and waiting to claw the alien off me, to falling asleep while watching the clock.
Stabelfeldt solves the mask issue by creating impressive custom-stitched headgear to keep his system running its best while maintaining the comfort he likes. Miller was having a hard time with her mask tugging when she changed positions at night, so her fiancé built a bedside CPAP shelf with an overhead hook for the mask when not in use.
As a quad with decreasing hand-function, I had a hard time adapting to the CPAP without being able to control it myself. I worked with an occupational therapist to create an oversized zip-tie-hoop handle for my mask, for my clumsy C4-5-ish hand to hook and yank away. With difficulty I got it to work in the therapy room but never had success at home. Thanks to my MS, those were my last days of hand function. The good news is by then I was normalizing use of the CPAP anyway, though it didn’t come easily.
In Space, No One Can Hear You Snore
Dr. Sankari emphasizes that sleep apnea is a very common, treatable condition, and CPAP can prevent worsening of SCI symptoms, while reducing the risk of decreased lifespan. Technology is making treatment more accessible and convenient than ever, with the rise of telehealth and at-home testing to replace the night in a sleep lab. “I don’t want [readers] to feel there are barriers,” Sankari says. “We’re going to break those barriers.”

Even after nine years of consistent use, I still haven’t got the fit and size of the mask completely down. The middle of my nose often looks raw and sore, but the payoff is entirely worth it. After my first full night with the CPAP, my daily 20-minute nap disappeared, and I haven’t had one since. Not to mention I no longer take my heart off-roading every night, or throw my wife into a panic wondering whether to start chest compressions. Slowly but surely, I graduated to long, peaceful nights and better, safer sleep.
When Miller began using a CPAP, it addressed harmful effects of sleep apnea she’d been suffering — nighttime gasping, morning headaches and chronic daytime exhaustion. Her message for anyone who is on the fence about getting treatment for their problem sleep: “Do not wait to go. Because I got to the point where I almost called 911.” She’s still working to use CPAP more consistently, but already she likes it enough to use it sometimes to breathe more easily when relaxing with a movie, and this summer she’s bringing it on the family camping trip to try it out in a cabin.
Stabelfeldt has trouble even imagining his life without the mask. “I would not even know how to do a night [without it],” he says. “If the BiPAP broke tonight, I would get back in my wheelchair and I would just stay in my wheelchair [until the BiPAP was fixed].”



Recent Comments
Abdul Mansour on Testing Two New Seat Designs That Will Let You Fly in Your Wheelchair
Alejandra on Adaptive Products Roundup: May 2026
Lisa Blinn on A Malpractice Case Against ParkingMD